Achillis Tendinities
Achilles tendinitis is an overuse injury of the Achilles (uh-KILL-eez) tendon, the band of tissue that connects calf muscles at the back of the lower leg to your heel bone.
Most commonly occurs in runners who have suddenly increased the intensity or duration of their runs. It’s also common in middle-aged people who play sports, such as tennis or basketball, only on the weekends.
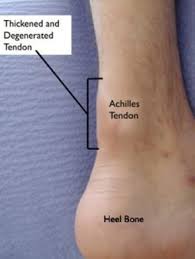
Symptoms:
The pain associated with Achilles tendinitis typically starts as a mild ache in the back of the leg or above the heel after running or other sports activity. Episodes of more-severe pain may occur after prolonged running, stair climbing or sprinting.

You might also experience tenderness or stiffness, especially in the morning, which usually improves with mild activity.
Causes of Achillis Tendinitis:
Achilles tendinitis is caused by repetitive or intense strain on the Achilles tendon, the band of tissue that connects your calf muscles to your heel bone. This tendon is used when you walk, run, jump or push up on your toes.
The structure of the Achilles tendon weakens with age, which can make it more susceptible to injury — particularly in people who may participate in sports only on the weekends or who have suddenly increased the intensity of their running programs.
Risk factors:
A number of factors may increase your risk of Achilles tendinitis, including:
Achilles tendinitis occurs most commonly in men.
Age. Achilles tendinitis is more common as you age.
Physical problems. A naturally flat arch in your foot can put more strain on the Achilles tendon. Obesity and tight calf muscles also can increase tendon strain.
Training choices. Running in worn-out shoes can increase your risk of Achilles tendinitis. Tendon pain occurs more frequently in cold weather than in warm weather, and running on hilly terrain also can predispose you to Achilles injury.
Medical conditions. People who have psoriasis or high blood pressure are at higher risk of developing Achilles tendinitis.
Medications. Certain types of antibiotics, called fluoroquinolones, have been associated with higher rates of Achilles tendinitis.
Complications:
Achilles tendinitis can weaken the tendon, making it more vulnerable to a tear (rupture) — a painful injury that usually requires surgical repair.
Prevention:
While it may not be possible to prevent Achilles tendinitis, you can take measures to reduce your risk:
Increase your activity level gradually. If you’re just beginning an exercise regimen, start slowly and gradually increase the duration and intensity of the training.
Take it easy. Avoid activities that place excessive stress on your tendons, such as hill running. If you participate in a strenuous activity, warm up first by exercising at a slower pace. If you notice pain during a particular exercise, stop and rest.
Choose your shoes carefully. The shoes you wear while exercising should provide adequate cushioning for your heel and should have a firm arch support to help reduce the tension in the Achilles tendon. Replace your worn-out shoes. If your shoes are in good condition but don’t support your feet, try arch supports in both shoes.
Stretch daily. Take the time to stretch your calf muscles and Achilles tendon in the morning, before exercise and after exercise to maintain flexibility. This is especially important to avoid a recurrence of Achilles tendinitis.
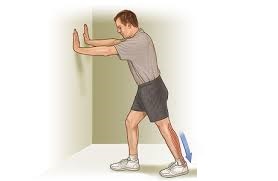
Strengthen your calf muscles. Strong calf muscles enable the calf and Achilles tendon to better handle the stresses they encounter with activity and exercise.
Cross-train. Alternate high-impact activities, such as running and jumping, with low-impact activities, such as cycling and swimming.
Diagnosis of Achillis Tendinitis:
During the physical exam, your doctor will gently press on the affected area to determine the location of pain, tenderness or swelling. He or she will also evaluate the flexibility, alignment, range of motion and reflexes of your foot and ankle.
Imaging tests:
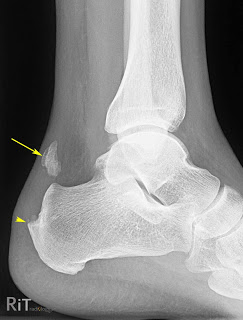
X-rays. While X-rays can’t visualize soft tissues such as tendons, they may help rule out other conditions that can cause similar symptoms.
Ultrasound. This device uses sound waves to visualize soft tissues like tendons. Ultrasound can also produce real-time images of the Achilles tendon in motion, and color-Doppler ultrasound can evaluate blood flow around the tendon.
Magnetic resonance imaging (MRI). Using radio waves and a very strong magnet, MRI machines can produce very detailed images of the Achilles tendon.
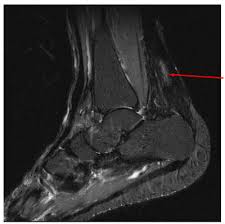
Treatment of Achillis Tendinitis:
Tendinitis usually responds well to self-care measures. But if your signs and symptoms are severe or persistent, your doctor might suggest other treatment options.
Medical Treatment:
If over-the-counter pain medications — such as ibuprofen (Advil, Motrin IB, others) or naproxen (Aleve) — aren’t enough, your doctor might prescribe stronger medications to reduce inflammation and relieve pain.
Physiotherapy treatment:
Physiotherapy is the treatment of a disease or condition by physical or mechanical means, such as through exercise or heat. A physiotherapist provides these treatments. He or she will also provide education, instruction, and support for recovery.
For an Achilles tendon injury, the following treatments are often used:
- Stretching and flexibility exercises. These are key to helping your tendon heal without shortening and causing long-term pain.
- Strengthening exercises. They will help you regain strength you might have lost while the tendon was healing. And they will help protect you from another injury.
- Ultrasound heat therapy. It improves blood circulation, which may aid the healing process.
- Deep massage. It helps you increase flexibility and blood circulation in the lower leg. It can also help prevent further injury.

A special type of strengthening called “eccentric” strengthening, involving a slow let down of a weight after raising it, has been found to be especially helpful for persistent Achilles problems.
Orthotic devices. A shoe insert or wedge that slightly elevates your heel can relieve strain on the tendon and provide a cushion that lessens the amount of force exerted on your Achilles tendon.
Surgery:
If several months of more-conservative treatments don’t work or if the tendon has torn, your doctor may suggest surgery to repair your Achilles tendon.
Self-care strategies include the following steps, often known by the acronym R.I.C.E. Principle:
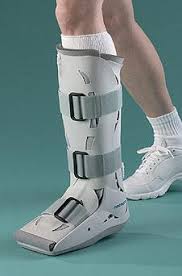
Rest. You may need to avoid exercise for several days or switch to an activity that doesn’t strain the Achilles tendon, such as swimming. In severe cases, you may need to wear a walking boot and use crutches.
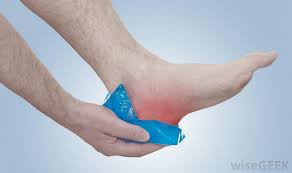
Ice. To decrease pain or swelling, apply an ice pack to the tendon for about 15 minutes after exercising or when you experience pain.
Compression. Wraps or compressive elastic bandages can help reduce swelling and reduce movement of the tendon.
Elevation. Raise the affected foot above the level of your heart to reduce swelling. Sleep with your affected foot elevated at night.
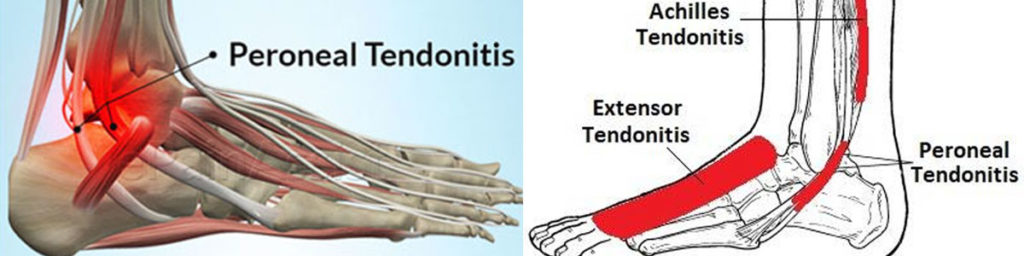
Related Other Article about Heel Pain :



8 Comments