Swan Neck Deformity: Physiotherapy Treatment
Introduction of Swan Neck Deformity
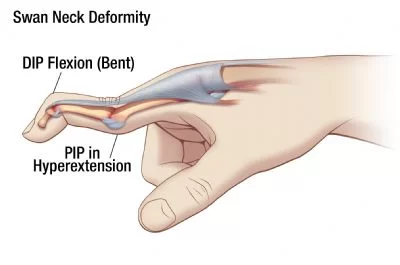
Swan neck deformity is a deformed position of the finger, in which the joint closest to the fingertip is permanently bent toward the palm while the nearest joint to the palm is bent away from it (DIP flexion with PIP hyper-extension). It is commonly caused by injury or inflammatory conditions like rheumatoid arthritis or sometimes familial (congenital, like Ehlers-Danlos syndrome.
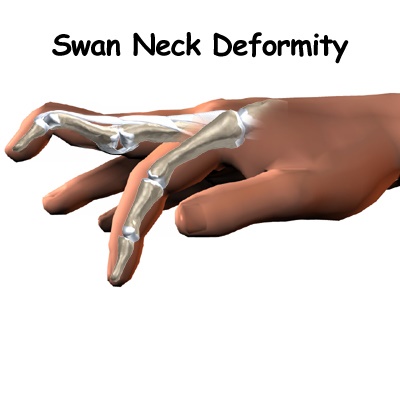
For a swan neck deformity to occur, abnormal stress must be put on the ligament around the PIP joint of the finger.
The stress causes the ligament to loosen, which then causes hyperextension of the PIP joint. As a result, the PIP joint bows in towards the palm.
Simultaneously, the joint furthest from the palm (DIP joint) forces the fingertip to point towards the palm.
The abnormally bent fingers may make it difficult for a person with swan neck deformity to grasp objects or make a fist. The limited motion may be classified as a disability, as the person has lost some fundamental functions of the fingers and hands.
Some similar finger malformations can be mistaken for swan neck deformity. These include the duckbill deformity, which causes the thumb or fingers to form a 90-degree angle.
Though related to other deformities, swan neck deformity is distinct in that it can only occur on the fingers, as the thumb lacks a middle joint.
Pathophysiology in swan neck deformity
This Deformity has many possible causes arising from the DIP, PIP, or even the MCP joints. In all cases, there is a stretching of the volar plate at the PIP joint to allow hyperextension, plus some damage to the attachment of the extensor tendon to the base of the distal phalanx that produces a hyperflexed mallet finger. Duckbill deformity is a similar condition affecting the thumb (which cannot have true swan neck deformity because it does not have enough joints).
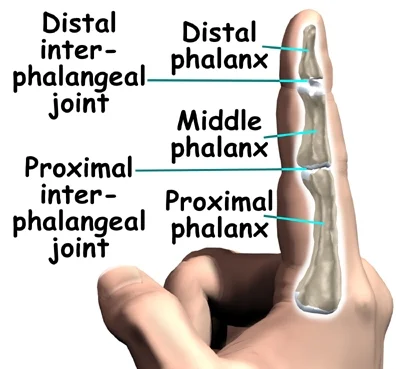
What are the Causes of Swan Neck Deformity?
While there are several potential causes of this deformity, the most common cause is rheumatoid arthritis.
other types of arthritis
untreated mallet finger – a condition often caused by injury
poorly healed fracture in the finger
other direct trauma to the finger that has weakened the ligaments surrounding the PIP joint
nerve damage that causes muscle spasms
severely jammed fingertip
tightened hand muscles due to injury
looseness of the fibrous plate inside the hand located at the base of the fingers
loose finger ligaments
ruptured finger tendon or tendons
some genetic conditions, such as Ehlers-Danlos syndrome
People diagnosed with rheumatoid arthritis are at greater risk for developing swan neck deformity in one or more of their fingers.
When first diagnosed with rheumatoid arthritis, a person may wish to talk to a doctor about precautionary measures to help avoid developing swan neck deformity as the disease progresses.
Which Symptoms are seen in Swan Neck Deformity?
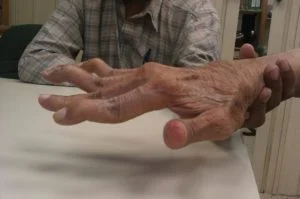
In the later stages of swan neck deformity, it is relatively easy to recognize symptoms visually.
Earlier signs of swan neck deformity may include pain when bending the knuckle and a slight bend in the wrong direction of one or more fingers.
Left untreated, the two outer joints of the finger will eventually bend noticeably, causing the finger to resemble a swan’s neck.
How Diagnosis is Done?
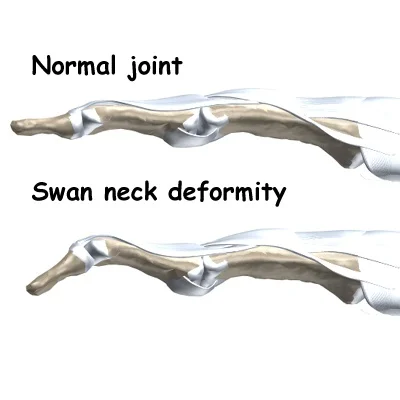
Doctors diagnose swan neck deformity with a visual examination of the hands. The doctor will look for a hyper-extended middle joint (PIP) and check whether the tip of the finger is flexing inwards to point towards the palm.
In addition to determining if a patient has a swan neck deformity, a doctor will look to diagnose the cause. For people with rheumatoid arthritis, the most likely cause is the arthritis.
Treatment of Swan Neck Deformity
There are a variety of treatment options for people who have swan neck deformity. There are two broad categories of treatment: surgical and non-surgical.
Non-Surgical Treatment
If rheumatoid arthritis is not the cause, a doctor may order an X-ray of the finger or fingers to determine if an acute injury may be the cause.
Non-surgical treatment focuses on restoring flexibility to the PIP joint and aligning the hand and fingers. Fixing the PIP joint should fix the DIP joint in most situations. If it does not, additional surgery may be required.
In some cases, a person may require physiotherapy Treatment.
Physiotherapy Treatment

Physiotherapy Treatment goals are mainly to improve range of motion, stretch exercise tight muscles, strengthen weak muscles and try to minimize deformity and relieve pain.
These treatments use stretching, massage, and joint mobilization to help restore the function and alignment of the fingers and hands.
Splints:
In addition to therapies or as a stand-alone treatment, a doctor may prescribe special finger splints. These produce the best results when the PIP joints are most supple. Many newer styles of splints resemble jewelry and can be discrete or decorative.
A person may take over-the-counter or prescription medicines to help reduce pain and discomfort. A person should consult their doctor before taking any new medications.
Surgical Treatment Options:
Before surgery, a surgeon may suggest that a person try some of the non-surgical treatment options for several weeks.
Severe cases of this deformity, as well as those that do not respond to therapies and splints, are the most likely to be recommended for surgery.
There are several surgical options available. Soft tissue surgery, finger joint fusion, and PIP joint arthroplasty are all viable options for treating swan neck deformity.
Soft tissue surgery involves releasing, aligning, and balancing the ligaments around the PIP joint. However, surgery that aims to fix the soft tissue that contributes to swan neck deformity may not be as effective. After surgery, most people will receive physical therapy to aid recovery.
Finger joint fusion involves fusing the DIP joint so that the fingertip will not be able to bend at the DIP joint. Fusing the DIP joint stabilizes the joint, reduces pain, and avoids further deformity. In more severe cases, a surgeon may recommend fusing the PIP joint in a slightly bent position.
PIP joint arthroplasty involves replacing part or all of the PIP joint in the affected fingers. Both ligament sections around the joint are removed and replaced. Once the new ligaments are in place, the surgeon typically reconstructs some of the soft tissue to help restore movement to the finger.
Recovery and management
After surgery, it is not uncommon for a person to undergo continued occupational and physical therapies. These therapies will help a person gradually regain strength and mobility in the fingers. Typical recovery times range from a few months to half a year.
The goal of therapy is to regain strength, improve range of motion, bring back fine motor skills, and reduce pain.
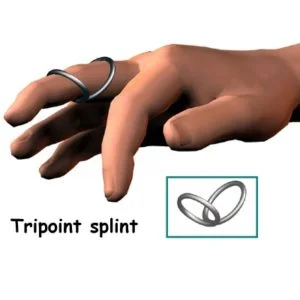
In addition to therapies, a person may continue to wear a brace or splint.
If this deformity occurred as a result of an acute injury, a person will probably experience no further complications once they recover from surgery.
People with rheumatoid arthritis may need to undergo surgery and therapy several times to reduce the impact of swan neck deformity.






5 Comments