Trigeminal Neuralgia
Trigeminal neuralgia is a chronic pain condition that affects the trigeminal nerve, which carries sensation from your face to your brain. If you have trigeminal neuralgia, even mild stimulation of your face — such as from brushing your teeth or putting on makeup — may trigger a jolt of excruciating pain.
You may initially experience short, mild attacks. But trigeminal neuralgia can progress and cause longer, more frequent bouts of searing pain. Trigeminal neuralgia affects women more often than men, and it’s more likely to occur in people who are older than 50.
Because of the variety of treatment options available, having trigeminal neuralgia doesn’t necessarily mean you’re doomed to a life of pain. Doctors usually can effectively manage trigeminal neuralgia with medications, injections, or surgery.
What are the Symptoms of Trigeminal Neuralgia?
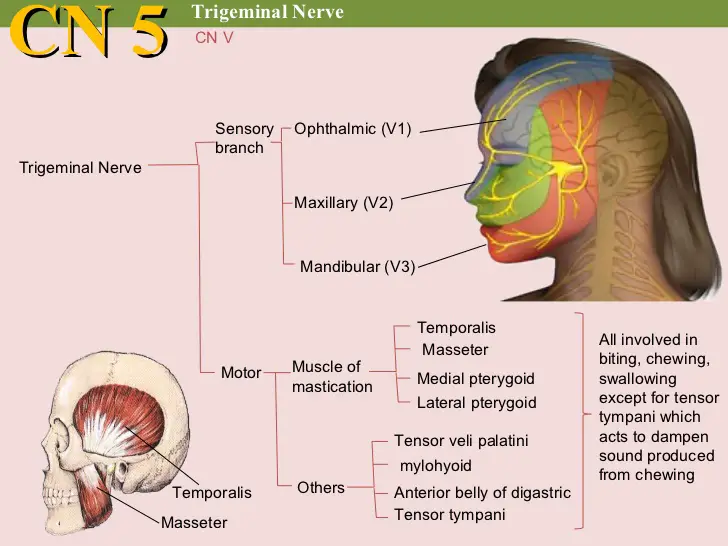
Illustration showing branches of the trigeminal nerve
Trigeminal neuralgia symptoms may include one or more of these patterns:
(1)Episodes of severe, shooting, or Tabbing pain that may feel like an electric shock
(2)Spontaneous attacks of pain or attacks triggered by things such as touching the face, chewing, speaking, or brushing teeth
Bouts of pain lasting from a few seconds to several minutes
(3)Episodes of several attacks lasting days, weeks, months, or longer — some people have periods when they experience no pain
Constant aching, burning feeling that may occur before it evolves into the spasm-like pain of trigeminal neuralgia
(4)Pain in areas supplied by the trigeminal nerve, including the cheek, jaw, teeth, gums, lips, or less often the eye and forehead
Pain affecting one side of the face at a time though may rarely affect both sides of the face
(5)Pain focused in one spot or spread in a wider pattern
What are the Causes of Trigeminal neuralgia?
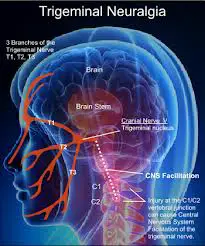
In trigeminal neuralgia, also called tic douloureux, the trigeminal nerve‘s function is disrupted. Usually, the problem is contact between a normal blood vessel — in this case, an artery or a vein — and the trigeminal nerve at the base of your brain. This contact puts pressure on the nerve and causes it to malfunction.
Trigeminal neuralgia can occur as a result of aging, or it can be related to multiple sclerosis or a similar disorder that damages the myelin sheath protecting certain nerves. Trigeminal neuralgia can also be caused by a tumor compressing the trigeminal nerve.
Some people may experience trigeminal neuralgia due to a brain lesion or other abnormalities. In other cases, surgical injuries, stroke, or facial trauma may be responsible for trigeminal neuralgia.
Diagnosis
In order to rule out other possible causes of facial pain, trigeminal neuralgia diagnosis requires a thorough medical history and physical examination. Your medical professional (typically a neurologist or primary care physician) will inquire about the type and frequency of pain, as well as what seems to trigger it and make it feel better or worse. Trigeminal neuralgia cannot be diagnosed with a single test; therefore, determining the type of pain is essential.
In addition, your physician might suggest imaging or lab work, including a CAT scan or a high-resolution MRI of the trigeminal nerve and its surrounding area. These tests can assist in determining if the pain is coming from an undetected case of multiple sclerosis or from a tumor or blood vessel anomaly. The physician may be able to determine where a blood vessel is pressing on a trigeminal nerve branch by using specific sophisticated MRI techniques.
Treatment of Trigeminal Neuralgia
The first line of treatment is medication.
The drug of choice is carbamazepine (Tegretol™), which eliminates or brings acceptable pain relief in 69 percent of patients.
Baclofen (Lioresal™) is the second drug of choice and may be more effective if used with low-dose carbamazepine.
Other medications that may be effective include pimozide, phenytoin (Dilantin™), capsaicin, clonazepam (Klonopin™), and amitriptyline (Elavil™).
Trigeminal Nerve Blocks
Injections at different points along the nerve (with a steroid drug or another substance) are known as nerve blocks, and they are used to lessen pain. They might offer those who suffer from trigeminal neuralgia some temporary pain relief. To get the desired alleviation, several injections are typically required, and each person will experience the effects for a varied amount of time.
Surgical procedures
(1) Percutaneous trigeminal radiofrequency rhizotomy
This procedure selectively destroys pain-causing nerve fibers while preserving touch fibers.
Lesioning techniques include radiofrequency thermocoagulation, glycerol injection, and mechanical trauma. They are used for patients who are poor candidates for major surgery.
Complications can include weakness in chewing, facial numbness, changes in tearing or salivation, and, less often, corneal ulcers, severe aching pain (anesthesia dolorosa), or meningitis.
(2) Microvascular decompression of the trigeminal nerve
This surgical technique involves microsurgery to move the vessel, causing compression away from the trigeminal nerve.
Relief is often long-lived; however, the incidence of facial numbness is much less than in selective rhizotomy and anesthesia dolorosa does not occur.
The procedure is best for patients younger than 65 with no significant medical or surgical risk factors.
Possible complications include aseptic meningitis, with head and neck stiffness; major neurological problems, including deafness and facial nerve dysfunction; mild sensory loss; cranial nerve palsy, causing double vision, facial weakness, and hearing loss; and, on very rare occasions, postoperative bleeding and death.
Microvascular decompression brings complete relief to 75 percent to 80 percent of patients. The recurrence rate is 5 percent to 17 percent.
Physiotherapy Treatment in Trigeminal Neuralgia
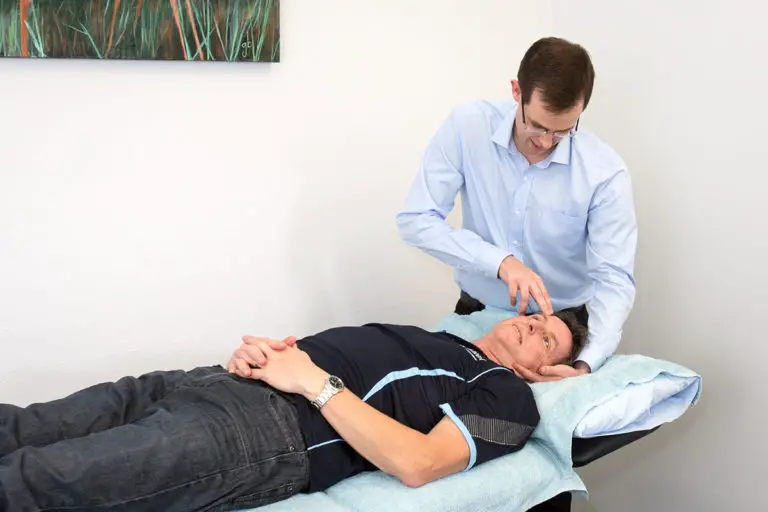
*The aims of Physiotherapy Treatment
To decrease pain and functional limitation, and to improve quality of life.
Treatments include the use of electro-physical agents to relieve pain during acute onset.
Manual therapy, exercise therapy for Temporomandibular Joint (TMJ) as well as self-massage for facial muscles can also help to restore patients’ functions.
Transcutaneous electrical nerve stimulation (TENS) currently is one of the
most commonly used forms of electroanalgesia
Interferential Therapy(IFT)
Interferential therapy (IFT) is another electro-physical modality commonly used for pain management in clinical situations. IFT is the application of alternating medium frequency current (4,000 Hz) with amplitude modulated at low frequency (0–250 Hz).
Several theoretical physiological mechanisms such as the gate-control theory, increased circulation, descending pain suppression, block of nerve conduction, and placebo have been proposed in the literature to support the analgesic effects of IFT reducing pain for patients with trigeminal neuralgia by having them receive fifteen sessions of IFT with treatment duration of thirty minutes.
The intensity of the impulse varied according to the patient’s tolerance. The results suggested that IFT could be considered as one of the electro-physical modalities in reducing pain for trigeminal neuralgia.
Acupuncture
In order to relieve pain, acupuncture inserts tiny needles along the “trigger points.” Acupuncture has been reported by some trigeminal neuralgia sufferers to lessen the severity and/or frequency of flare-ups.
For those seeking additional treatment following surgery or more natural approaches to treating trigeminal neuralgia, there are also options such as meditation, wellness centers, and lifestyle modification programs.
Care of Trigeminal Neuralgia
The pain and anxiety associated with trigeminal neuralgia, while not life-threatening, can significantly impair the quality of life for both the affected individual and those in their vicinity. The first steps to providing care for a loved one with trigeminal neuralgia are to acknowledge the extent of the pain the individual is experiencing and to be understanding. Additional actions could be:
- assisting your loved one in taking their prescriptions as prescribed and keeping you informed about the treatment’s progress.
- promoting medical appointments and looking at alternate forms of care when prescription drugs run out.
- assisting in locating and scheduling visits with physicians who are able to provide evaluations and second opinions.
It is crucial to collaborate closely with knowledgeable and caring medical professionals who can assist in determining the most effective therapeutic strategy for each individual.
When to Consult a Doctor?
See your doctor if you have facial pain, especially if it is persistent, recurrent, or not helped by over-the-counter medications.
FAQ
What can cause trigeminal neuralgia?
Pressure on the trigeminal nerve around its entry point into the brain stem results in classical trigeminal neuralgia. The lowest region of the brain where it joins the spinal cord is called the brain stem. The trigeminal nerve is usually compressed or crushed by an artery or vein, which results in pressure.
Is trigeminal neuralgia curable?
Trigeminal neuralgia can increase over time if treatment is not received, but attacks may start out moderate and brief. While there isn’t always a cure for trigeminal neuralgia, there are techniques to lessen the excruciating agony. Anticonvulsive drugs are typically the initial line of treatment.
What is the best treatment for neuralgia?
Your doctor will typically prescribe medication to reduce or block the pain signals that are sent to your brain in order to treat trigeminal neuralgia. drugs that prevent seizures. Trigeminal neuralgia is typically treated with carbamazepine (Tegretol, Carbatrol, and other brands), which has been demonstrated to be successful in treating the condition.
Can you live a normal life with trigeminal neuralgia?
Trigeminal neuralgia can be very challenging to live with and can have a major negative impact on quality of life. To prevent inciting discomfort, you could feel like skipping meals, showers, or shaving. Additionally, your fear of pain might make you avoid social situations.
Is trigeminal neuralgia harmful?
One of the most excruciating neurological disorders, trigeminal neuralgia is frequently compared as a “lightning bolt” that has become lodged in one’s face or a stabbing feeling there. Indeed, the sufferer is rendered completely helpless by these brief bursts of excruciating pain, which happen often during the day.





3 Comments