Leprosy and physiotherapy management
DEFINITION OF LEPROSY :
1: A chronic infectious disease caused by a mycobacterium (Mycobacterium leprae) affecting especially the skin and peripheral nerves and characterized by the formation of nodules or macules that enlarge and spread accompanied by loss of sensation with eventual paralysis, wasting of muscle, and production of deformities — called also Hansen’s disease
2: A morally or spiritually harmful influence first system recognizes two types of leprosy: tuberculoid and lepromatous. A person’s immune response to the disease determines their type of leprosy.
The immune response is good and the disease only exhibits a few lesions (sores on the skin) in tuberculoid leprosy. The disease is mild and only mildly contagious.
The immune response is poor in lepromatous leprosy and affects the skin, nerves, and other organs. There are widespread lesions and nodules (large lumps and bumps). This disease is more contagious.
WHO categorizes the disease based on the type and number of affected skin areas. The first category is paucibacillary, in which five or fewer lesions with no bacteria are detected in the skin sample. The second category is multibacillary, in which there are more than five lesions, bacteria detected in the skin smear or both.
CLASSIFICATION OF LEPROSY
Clinical studies use the Ridley-Jopling system. It has six classifications based on the severity of symptoms. They are:
1. Intermediate leprosy: a few flat lesions that sometimes heal by themselves and can progress to a more severe type
2. Tuberculoid leprosy: a few flat lesions, some large and numb; some nerve involvement; can heal on its own, persist, or may progress to a more severe form.
3. Borderline tuberculoid leprosy: lesions similar to tuberculoid but smaller and more numerous; less nerve enlargement; may persist, revert to tuberculoid, or advance to another form.
4. Mid-borderline leprosy: reddish plaques, moderate numbness, swollen lymph glands; may regress, persist, or progress to other forms.
5. Borderline lepromatous leprosy: many lesions including flat lesions, raised bumps, plaques, and nodules, sometimes numb; may persist, regress, or progress.
6. Lepromatous leprosy: many lesions with bacteria; hair loss; nerve involvement; limb weakness; disfigurement; doesn’t regress.
TRANSMISSION OF LEPROSY
Leprosy spreads through contact with the mucus of an infected person. This usually occurs when the infected person sneezes or coughs. The disease isn’t highly contagious. Close, repeated contact with an untreated person can lead to contracting leprosy.
The bacteria responsible for leprosy multiply very slowly. The disease has an incubation period (the time between infection and the appearance of the first symptoms) of up to five years. Symptoms may not appear for as long as 20 years.
According to the New England Journal of Medicine, an armadillo native to the southern United States can also carry and transmit the disease to humans.
LEPROSY SYMPTOMS
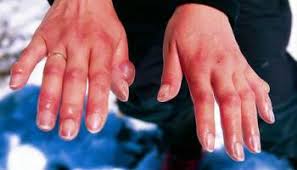
Symptoms mainly affect the skin, nerves, and mucous membranes (the soft, moist areas just inside the body’s openings).
The disease can cause skin symptoms such as:
A large, discolored lesion on the chest of a person with Hansen’s disease.
A large, discolored lesion on the chest of a person with Hansen’s disease.
Discolored patches of skin, usually flat, that may be numb and look faded (lighter than the skin around)
Growths (nodules) on the skin
Thick, stiff, or dry skin
Painless ulcers on the soles of feet
Painless swelling or lumps on the face or earlobes
Loss of eyebrows or eyelashes
Symptoms caused by damage to the nerves are:
Numbness of affected areas of the skin
Muscle weakness or paralysis (especially in the hands and feet)
Enlarged nerves (especially those around the elbow and knee and in the sides of the neck)
Eye problems that may lead to blindness (when facial nerves are affected)
Enlarged nerves below the skin and dark reddish skin patch overlying the nerves affected by the bacteria on the chest of a patient with Hansen’s disease. This skin patch was numb when touched.
Enlarged nerves below the skin and dark reddish skin patch overlying the nerves affected by the bacteria on the chest of a patient with Hansen’s disease. This skin patch was numb when touched.
Symptoms caused by the disease in the mucous membranes are:
A stuffy nose
Nosebleeds
Since Hansen’s disease affects the nerves, loss of feeling or sensation can occur. When loss of sensation occurs, injuries such as burns may go unnoticed. Because you may not feel the pain that can warn you of harm to your body, take extra caution to ensure the affected parts of your body are not injured.
If left untreated, the signs of advanced leprosy can include:
Paralysis and crippling of hands and feet
Shortening of toes and fingers due to reabsorption
Chronic non-healing ulcers on the bottoms of the feet
Blindness
Loss of eyebrows
Nose disfigurement
Other complications that may sometimes occur are:
Painful or tender nerves
Redness and pain around the affected area
Burning sensation in the skin
LEPROSY DIAGNOSIS :
The diagnosis of leprosy is often established from the patient’s clinical signs and symptoms. A careful skin exam and neurologic exam will be undertaken by a healthcare professional. If a laboratory is available, skin smears or skin biopsies may be obtained for a more definitive diagnosis. Skin smears or biopsy material that show acid-fast bacilli with the Ziel-Neelsen stain or the Fite stain can diagnose multibacillary leprosy. If bacteria are absent, paucibacillary leprosy can be diagnosed. Other less commonly used tests include blood exams, nasal smears, and nerve biopsies. Specialized tests can be done to place the patient in the more detailed Ridley-Jopling classification.
PREVENTION OF LEPROSY
Early detection of the disease is important, since physical and neurological damage may be irreversible even if cured. Medications can decrease the risk of those living with people with leprosy from acquiring the disease and likely those with whom people with leprosy come into contact outside the home. However, concerns are known of resistance, cost, and disclosure of a person’s infection status when doing follow-up of contacts. Therefore, the WHO recommends that people who live in the same household be examined for leprosy and treated only if symptoms are present.
The Bacillus Calmette–Guérin (BCG) vaccine offers a variable amount of protection against leprosy in addition to its target of tuberculosis. It appears to be 26 to 41% effective (based on controlled trials) and about 60% effective based on observational studies with two doses possibly working better than one. The development of a more effective vaccine is ongoing.
SELF-CARE AT HOME FOR LEPROSY
Prescribed antibiotics medications are the primary treatment for leprosy. Compliance with the full course of antibiotics is crucial to successful treatment.
Patients should also be educated to closely inspect their hands and feet for possible injuries sustained which may go unnoticed because of the loss of sensation.
1. Ulcers or tissue damage can result, leading to skin infections and disability.
2. Proper footwear and injury prevention should be encouraged.
LEPROSY TREATMENT
Leprosy is a curable disease using the highly effective MDT (multidrug therapy).
In 1981, a World Health Organization Study Group recommended multidrug treatment with three medications: dapsone, rifampicin (Rifadin), and clofazimine (Lamprene).
This long-term treatment regimen cures the disease and prevents the complications associated with leprosy if started in its early stages.
The National Hansen’s Disease Program (NHDP) currently recommends different treatment regimens for patients with tuberculoid and lepromatous leprosy.
NHDP recommendations:
- Tuberculoid leprosy:
Twelve months of treatment using rifampin and Dapsone daily
2. Lepromatous leprosy
Twenty-four months of treatment using rifampin, dapsone, and clofazimine daily
The WHO recommended therapy for leprosy is given significantly shorter and less often, as this treatment policy is based upon practical considerations in countries with fewer medical resources. However, the relapses with treatment according to the WHO recommendations are significantly greater than those with the NHDP recommended therapy.
Individuals who develop type 1 or type 2 reactions may require other medications.
Type 1 reaction (reversal reaction):
Treatment may include the use of corticosteroids, salicylates, and nonsteroidal anti-inflammatory drugs (NSAIDs).
Type 2 reaction (ENL):
Treatment may include the use of corticosteroids, salicylates, NSAIDs, clofazimine, and thalidomide (Thalomid).
SURGICAL TREATMENT FOR LEPROSY
There are various surgical procedures available for certain patients with leprosy. These surgical procedures are aimed at restoring the function of affected body parts (for example, correcting clawed hand deformities) and to cosmetically improving areas damaged by the disease. Amputation of affected body parts is sometimes necessary. Surgery may also be necessary to drain a nerve abscess (pus collection) or to relieve the compression of nerves.
Some patients with leprosy may require psychological counseling, physical therapy, and occupational therapy.
DEFORMITIES IN LEPROSY:
Deformities occurring in leprosy:
1 Nose deformities
2. Face Deformities
3. Mask face, faces leonina, sagging face, lagophthaimos, loss of eye brows (supercilliary madorosis and eyelashes (ciliary madarosis),
4. ulcers and opacities, perforated nose, depressed nose, ear deformities, e.g. nodules on the ear and elongated lobules.
5. Hands Deformities:
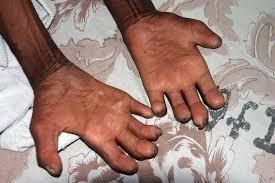
Claw hand, wrist drop, ulcers, absorption of digits, thumb–web contracture, hollowing of the interosseous spaces, and swollen hand.
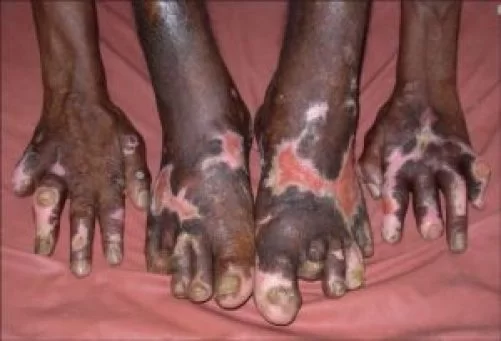
6. Feet Deformities
Planter ulcer, foot drop, inversion of the foot, clawing of the toes, absorption of the toes, collapsed foot, swollen foot, and callosities.
7. Other Deformities
Gynecomastia and perforation of the palate. All along it has commonly been believed that it is highly contagious and incurable. Even today, in spite of scientific information available about leprosy, it is deeply rooted in the minds of most people at all levels of society, with the result that social ostracism is apparent everywhere. This has led patients to hide their early lesions, and thereby delay treatment just at the period when they could be most speedily cured. Failure to appreciate the importance of social and psychological factors has resulted in the failure of otherwise well-conceived programs.
GOALS OF PHYSIOTHERAPY FOR NON-SURGICAL PATIENTS OF LEPROSY DISEASE :

The major aim is to prevent or reduce complications, deformity, and disability in the body through Physiotherapy.
Means
The ways of reaching these Goals are-
By teaching the patient.
By treating and helping the patient.
Teachings
What the disease of leprosy is?
The possible complications and deformities resulting from leprosy.
prevention of complications, deformities and disabilities.
Treating and Helping
To respect themselves enough to take medication regularly and to take care of complications.
To protect their own anesthetic hands, feet, and eyes.
To keep their skin soft and supple.
To keep their joints flexible.
To preserve all possible movements of hands and feet.
To keep their muscles strong.
To use their hands, feet, and eyes safely, in daily work.

GOALS OF PHYSIOTHERAPY FOR SURGICAL PATIENTS OF LEPROSY:
To protect and prevent further damage and deformity.
To improve and restore function.
To improve the appearance of hands, feet, face, and eyes.
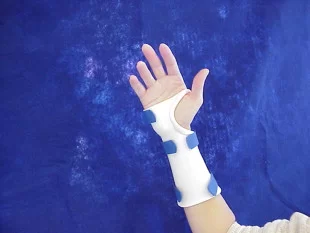
LEPROSY AND SPLINT FOR HAND
Surgical Techniques Used in Leprosy Disease
Tendon Transfer: Moving the distal end of the tendon to a new place so that contraction of muscle belly will produce needed movements used to replace paralyzed muscles. Example- Transfer of forearm muscle to make finger movements.
Tendon Lengthening: Lengthening the tendon of a muscle to permit more movement and reduce contracture. Example- Tendo Calcaneus lengthening.
Capsulotomy: To loosen tight joint capsule often done with tendon lengthening and tendon transfer to improve range of motions. Tighten the loose joint capsule using a suture.
Arthrodesis: Elimination of unstable and deformed joints.
Tenodesis: Attach a piece of tendon across the joint to reduce the movement. The tendon then acts as a ligament. Example- Tenodesis of MCP joint to prevent hyperextension.
Physical Therapy Goals:
To increase and regain range of motion.
Improve muscle strength, particularly in muscles to be transferred.
Clean supple skin in areas of surgery.
Teach home self-care.
Protect tissue during wearing.
Prevent/reduce swelling.
Muscle re-education after tendon transfer.
Safe use of any new restored skill in work.
PHYSIOTHERAPY TREATMENT:
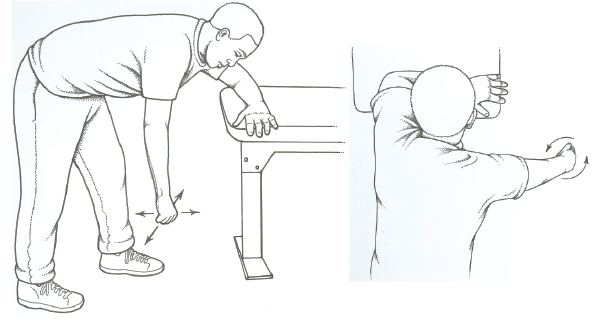
For increasing/regaining ROM: ROM can be increased by soaking the skin or part in warm water and then performing passive movement to the part affected.
To improve strength, especially in tendon transfer: Active exercise in all parts in which surgery is performed.
Clean supple skin: It is provided by soaking the part in soap water, rubbing off thick skin, oiling, self-massage, and protecting the part from infection.
Home care: teaching skin, hand, foot, and eye care to groups and individuals and teaching the patients actual home care.
Protect tissue during healing: Rest, body position, and POP cast.
Prevent/Reduce swelling: Elevation, active and passive exercise.
Muscle Re-education after tendon transfer: Teaching new restored skills in movements provided by tendon transfer.
Self-restored skills in daily work: Teaching patients to use any new skill safely in specific tasks. Providing hand, eye, and foot protection.





3 Comments