Bone Tuberculosis
Mycobacterium tuberculosis is a highly contagious bacteria that causes tuberculosis, an illness spread through the air. It can pass through the blood to the spine, joints, lymph nodes, and bones.
A serious infectious disease that typically affects the lungs is tuberculosis. Skeletal TB is the term used when it affects your bones.
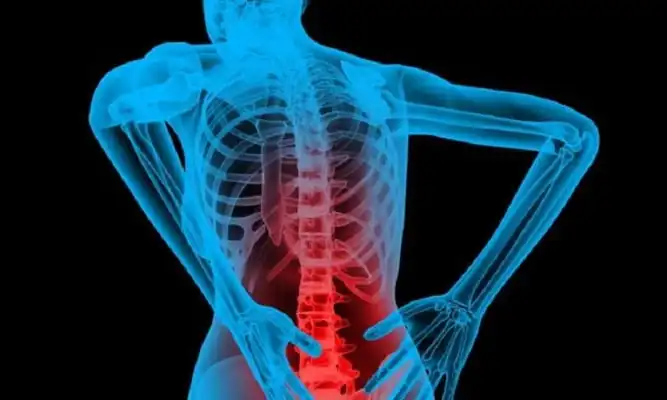
A collection of serious viral diseases known as “bone TB” have caused more misery in the past 20 years, particularly in the world’s developing nations. This leads to the development of abscesses and stiffness in the impacted joints. Hip and knee joints are badly affected by bone TB. For AIDS patients, it is an additional illness. Osteoarticular symptoms are prevalent in tuberculosis cases. It hurts in the trochanteric region, in the extraspinal skeleton, or in a prosthetic joint.
In most cases, bacilli that are stuck in the bone reactivate to cause bone TB. During the initial stage of mycobacteria infection, the abundant vascular supply of the vertebra or the development plates of the long bones causes bacillus to affect the spine and major joints. Bone TB, also known as ART, is the outcome of an initial infection that spreads from the bone to the joint.
What Kinds of Tuberculosis Are There?
TB primarily comes in two forms:
- Pulmonary tuberculosis: tuberculosis that primarily affects the lungs. Breathing problems, chest pain, and other lung-related conditions are some of the symptoms of bone TB that you might encounter. Primarily affecting the lungs. Lung issues, breathing difficulties, and chest pain can all be caused by the infection.
- Extrapulmonary tuberculosis: tuberculosis that travels outside of the lungs to other parts of the body. This is more prevalent in people with weakened immune systems, which is mostly brought on by HIV/AIDS. Additionally, extrapulmonary TB can infiltrate the bones, leading to an uncommon and deadly case of bone TB. When tuberculosis affects parts of your body other than your lungs, it is known as extrapulmonary tuberculosis. This is more common in those with HIV/AIDS-related immune system deterioration.
Types of bone TB
One kind of extrapulmonary TB is bone TB, also known as osteoarticular TB. Although it can also spread to other bones and joints, bone TB most commonly affects the spine.
In most cases, bacilli that are lodged in the bone reactivate to cause bone TB. During the initial stage of mycobacteria infection, the abundant vascular supply of the vertebra or the growth plates of the long bones causes bacillus to affect the spine and large joints. Bone TB, also known as ART, is the result of an initial infection that spreads from the bone to the joint.
Different types of bone TB can be treated using different methods, and there are several categories of bone TB. Here are a few of the types in the joint :
- Spine tuberculosis
- TB affecting the hip joint
- TB affecting the elbow joint
- TB affecting the knee joint
- TB affecting the ankle joint
- TB affecting the upper limbs
The most prevalent kind is TB of the spine. When the mycobacterium infection gets into your spinal cord, this is what happens. Another name for spinal tuberculosis is Pott’s disease.
Bone Tuberculosis Causes
Mycobacterium tuberculosis is another cause of skeletal tuberculosis. Research indicates that bone or spinal tuberculosis may not be airborne, in contrast to pulmonary TB. If you come into contact with the bodily fluids or pus of an infected person, the infection may spread through your blood.
Pulmonary tuberculosis can also lead to skeletal tuberculosis. Through blood vessels, mycobacteria can readily travel from your lungs to your bones, spine, or joints. Your spinal vertebrae or long bones may be impacted by this.
This kind of tuberculosis is uncommon and is usually found in areas where AIDS infections are pervasive. AIDS patients are more susceptible to bone tuberculosis because the virus compromises their immune system.
When tuberculosis (TB) penetrates your bones instead of just your lungs, it becomes known as bone TB. Airborne particulates frequently spread it. Once contracted, the tuberculosis infection can travel through your bloodstream from your lungs to your bones or joints. The onset of bone tuberculosis frequently occurs in the dense blood supply located in the center of long bones.
Even though bone tuberculosis is uncommon, it has increased recently in developing nations, primarily due to the spread of AIDS in these areas. If you don’t start taking your medication as soon as possible and treat bone TB for an extended period of time, you may experience major complications.
There have been fewer cases of bone tuberculosis in recent decades due to a significant increase in treatment prevalence. The following are the main reasons for developing a bone TB infection:
Tuberculosis: It is the cause of tuberculosis. It can harm lymph nodes, the thymus, and even bones when it enters the human body.
Transmission: Since tuberculosis is an infectious disease, it travels quickly through the air from person to person.
Inadequate care: If a patient with tuberculosis (TB) or any other type of TB is not treated properly from the start, the bacteria will spread to the long bones’ plentiful vascular supply and cause bone TB.
Risk Factor
Individuals with compromised immune systems are more susceptible to tuberculosis (TB) development. Babies and those suffering from the following ailments are included in this:
- diabetes type 2
- HIV
- drug abuse disorder
- lung condition known as silicosis, which is brought on by breathing in tiny silicon particles
- cancer of the head and neck
- grave renal illness
- the low mass of the body
The immune system may also be weakened by some medical procedures, including:
- corticosteroid
- specific drugs for Crohn’s disease and rheumatoid arthritis
- transplanting organs
Individuals with HIV or low vitamin D levels are more susceptible to certain forms of bone TB Trusted Source. The body’s capacity to stop the TB bacteria from spreading throughout the body is impacted by these ailments.
Symptoms of Bone TB
Bone TB symptoms usually develop gradually over weeks, months, or even years. Among the symptoms are:
- discomfort and soreness surrounding the injured bone
- loss of function in the vicinity of the injured bone or difficulty moving joints
- edema surrounding the bone
- muscle waste
- joint malformation
- abnormality of the bones
- fever
- sweats at night
- inexplicable drop in weight
- excruciating back discomfort
- Joint or back inflammation
- Inflexibility
- difficulty walking or moving, particularly in kids
- Abscess in the spine
- Swelling of soft tissues
- illnesses of the nerves
- Meningitis linked to tuberculosis
- Weakness in muscles
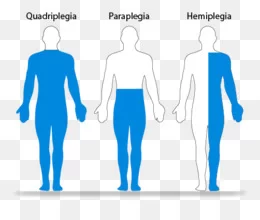
- Paraplegia is the paralysis of all four limbs, while tetraplegia is the paralysis of a single organ.
- Known by the name “hunchback,” kyphosis
- Deformities of the bones or spine
- Bone Tub Diagnosis
Bone TB usually affects one area of the body, though it can affect more than one. Bone TB can affect any bone or joint in a person. Nonetheless, the spine and weight-bearing joints are more frequently affected.
Bone TB symptoms differ from those of tuberculosis in general. A person may exhibit symptoms of bone TB, general TB, or both. The location of the TB in a person’s body determines the symptoms.
Symptoms of generalized tuberculosis include:
- feeling ill or feeble
- fever
- appetite decline
- sweats at night
- reduction in weight
- spitting
- spitting blood in the cough
- chest discomfort
Diagnosis of Bone TB
The following are typical techniques for identifying bone TB:
Cultivation of bacteria.
A lung infection is most likely the underlying cause of bone tuberculosis. To check for Mycobacterium tuberculosis, your doctor might draw blood or sputum samples.
Testing for the presence of bacteria in the body is the first step in diagnosing bone TB. Blood tests and skin tests can be used for this.
A tiny amount of tuberculin is injected under the skin (usually on the forearm) in the Mantoux tuberculin skin test. Following 48 to 72 hours, the region is assessed. A medical professional measures the bump in millimeters (mm) if the patient has a raised, hard bump on their skin. A provider determines whether a patient had a positive reaction by taking into account the size of the bump and the patient’s risk factors.
Autopsy
A biopsy is a procedure used by your doctor to remove a sample of infected tissue and examine it for infection.
Bodily fluid analysis
The fluid that surrounds and shields your lungs, called pleural fluid, may be drawn by your doctor to check for infections. They might also remove cerebrospinal fluid from the area surrounding your spinal cord. Your doctor might take joint or synovial fluid for testing if you have bone or joint tuberculosis.
If you have an infection, it’s possible that your doctor will remove a sample of extra fluid from the surrounding tissues of your lungs. It’s also possible that your doctor will remove some of the fluid surrounding your joints for additional testing if there is a suspicion of bone TB.
PCR test, or polymerase chain reaction
It is also possible to use PCR to test the samples that your doctor collects. This test increases the mycobacterium’s genetic makeup and aids in the detection of infection in trace amounts of fluid.
Additionally, the samples your doctor takes from you can be analyzed using PCR. This test amplifies the genetic material of the mycobacterium, enabling the detection of infection from extremely small fluid volumes.
Tests related to immunity
Your blood or bodily fluid sample can be used by your doctor to test for antibodies against AIDS or, in certain situations, tuberculosis.
Radiological examinations
An X-ray, CT scan, or MRI might be necessary if you have symptoms such as bone deformities.
It could be challenging for medical professionals to diagnose bone TB. This is a result of the long latency period associated with bone TB symptoms.
Typically, physicians identify bone TB by:
- examining a person’s medical complaints, such as pain
- examining specimens, as in the case of a TB blood test
- checking for the bacteria M. tuberculosis
Several tests can be used by medical professionals to diagnose tuberculosis (TB), including
either a blood test, a skin test, or both.
Both might be required if:
- A skin test yields positive results.
- There’s a possibility that the skin test resulted in a false negative.
If you haven’t had TB exposure for more than eight weeks or if your immune system isn’t functioning correctly, you may receive a false negative result.
Skin examination
If you have acquired tuberculosis bacteria, your physician may perform a purified protein derivative (PPD) skin test to find out.
In order to perform this test, the physician will inject 0.1 mL of PPD, or a tiny quantity of protein, beneath the epidermis. You’ll go back to your physician’s office to have the results examined two or three days later.
A positive outcome could be defined as a skin welt larger than five millimeters (mm) at the injection site of PPD. According to risk factors, health, and medical history, reactions that range in size from 5 to 15 mm may be regarded as positive. Regardless of risk factors, all reactions larger than 15 mm are regarded as positive.
However, the test is not flawless. It cannot determine whether you have active TB disease; it can only determine whether you have a TB infection. Furthermore, some individuals with TB do not react to the test. Some people pass the test and don’t have tuberculosis. Even if a person has recently received the TB vaccine, they may test positive for the disease.
Blood examination
To monitor the results of the TB skin test, your doctor may order a blood test. If you currently have a medical condition that might influence how you react to the skin test, they might also advise getting a blood test done first.
T-Spot and Quantiferon are the two TB blood tests that are currently authorized in the United States. The outcome of a blood test can be positive, negative, or unclear. The blood test, like the skin test, is unable to determine whether you have active tuberculosis.
Additional examinations
To check for TB bacteria, your doctor can perform tests on mucus or sputum that has been removed from deep within your lungs. You can spread the TB bacteria to other people if your sputum test comes back positive. Until your sputum tests negative for tuberculosis and you have begun treatment, you will need to wear a special mask.
If the results of previous tests are still unclear, you might require additional testing, such as a lung biopsy, bronchoscopy, or CT scan of the chest.
Are You Concerned That You May Have Bone TB Symptoms?
Make an online appointment for a Bone TB Test with Metropolis India to speak with one of our medical professionals.
With Metropolis India, you can have a hassle-free and seamless medical journey.
How does bone TB appear?
When bone TB is far more advanced, it can be difficult to diagnose the illness. Early-stage bone TB (spinal TB in particular) is painless, and the patient may not be displaying any symptoms, making diagnosis difficult. Upon final diagnosis, signs and symptoms of bone TB are typically quite advanced.
Moreover, the illness may occasionally lie dormant in the lungs and spread without the patient’s awareness, leaving them completely immune to tuberculosis.
Nevertheless, following a patient’s infection with bone TB, there are a few signs to be aware of:
- Acute back pain
- Stiffness
- Swelling
- Abscesses
Some harmful signs of more advanced bone tuberculosis include:
- Neurological issues
- Paralysis or paraplegia
- Limb shortening in young people
- Abnormalities of the bones
Additionally, individuals with bone TB may or may not exhibit the typical signs and symptoms of tuberculosis, such as:
- Exhaustion
- Fever
- Sweats at night
- Reduction in weight
Treatment of Bone Tuberculosis:
Although bone TB can have unpleasant side effects, the damage can be repaired if it is detected early and treated with the appropriate medication regimen.
Early intervention can stop tuberculosis from progressing and leading to problems, like loss of joint function or deformity.
Medical practitioners typically use a combination of anti-TB drugs, including chemotherapy, to treat bone TB.
For at least six months, doctors will prescribe antibiotics to a patient who also has tuberculosis in their lungs or throat. In certain cases of bone TB in the spine, doctors may operate.
Healthcare practitioners can use the Bacillus Calmette-Guerin (BCG) vaccine to vaccinate individuals against tuberculosis (TB).
Nonetheless, due to the minimal chance of contracting TB bacteria, US health authorities do not typically advise the BCG vaccination. When prescribing TB treatment, doctors may find that the BCG vaccine causes complications with certain tests.
Surgery:
To treat the severe condition, spinal surgery is required. This involves removing a portion of the vertebrae, a procedure known as a laminectomy.
Medication:
The first line of treatment for bone TB is medication, which can be taken for a maximum of six to eighteen months.
- isoniazid
- ethambutol
- pyrazinamide
- rifampin
- rifapentine
Although bone tuberculosis can have some severe side effects, the disease’s damage is typically reversible if it is detected early and treated with the appropriate medication regimen.
Spinal surgery, such as a laminectomy (where a portion of the vertebrae is removed), is frequently required.
Preventive measures include:
cigarettes, excessive alcohol intake, refined goods, and greasy foods like chicken, chips, onions, and other fried or highly saturated fat foods.
MDR-Therapy:
This treatment combines antitubercular medications with various pharmacological actions. The best course of action for treating bone TB is MDR.
DOTS therapy:
The “directly observed treatment short course,” or DOTS, approach suggests bone TB therapy, which entails a list of all the medications that fall under the category of antitubercular drugs.
XDR – TB:
Another name for it is extensively drug-resistant tuberculosis. It contains every rug that is resistant to M. tuberculosis, the causative agent. It includes all second-line medications. For the procedure, it contains medications such as polypeptides, thiazides, aminoglycosides, and para-aminosalicylic acid.
Immunizations
The BCG vaccine, which prevents tuberculosis, is primarily administered in nations where the disease is highly prevalent. Children respond better to this vaccine than adults do.
The United States does not use it extensively because the risk of tuberculosis is still minimal. Additionally, the vaccine may tamper with TB skin tests, leading to a false-positive result.
How does tuberculosis look in the future?
If a patient follows all medication instructions and has access to quality medical care, the treatment of tuberculosis can be successful.
Treatment for active TB can grow more challenging if the patient also has other medical conditions. For example, HIV compromises the body’s ability to defend itself from TB as well as additional infections by interfering with the immune system.
A tuberculosis infection may also become more complicated due to other infections, illnesses, and medical conditions, as well as inadequate access to care. The best chance of curing tuberculosis (TB) is typically provided by early detection and treatment, which includes a full course of antibiotics.
In what ways can tuberculosis be avoided?
It never hurts to know what steps you can take to avoid coming into contact with the TB bacteria or spreading the infection to others, even if your area has a low risk of tuberculosis.
TB Prevention
In North America, there is very little chance of coming into contact with TB bacteria. Nevertheless, understanding how to avoid it in high-risk situations is still crucial.
Among the crucial actions you can perform are:
- Arranging a test with a medical practitioner if you think you may have been exposed to tuberculosis
- Obtaining a TB test if you’re suffering from HIV or any other illness that raises your risk of infection
- Consulting a travel clinic or speak with your physician about getting tested both before and after visiting a nation with a high TB infection rate
- Enquiring about your workplace’s prevention and management of infections program and taking the recommended safety measures if your job exposes you to tuberculosis
- Keeping a distance from people who are actively tuberculosis infected if possible
Stopping the spread
If they don’t take precautions, individuals who have active TB can infect 10 to 15 people annually through close contact with the bacteria that triggers the infection, according to the WHO Trusted Source.
These actions can assist in stopping the spread of tuberculosis:
- If you believe that you might have been infected or exposed to tuberculosis or if your risk is higher, get tested.
- If you have latent or active tuberculosis, take all of the recommended medication.
- Avoid crowded areas and avoid contact with people until you are no longer contagious if you have been diagnosed as having active tuberculosis.
- If you have an active tuberculosis and must interact with people, wear a mask.
- Observe any additional guidelines your physician may provide you.
FAQs
How Significant Is Tuberculosis?
Although it is uncommon, the prevalence of this illness has increased in developing countries over the past few decades, primarily as a result of the spread of AIDS. This is true even though bone tuberculosis is an extremely rare illness. Untreated bone tuberculosis can lead to a variety of grave consequences and is infamously difficult to diagnose.
How long will it take for your bone TB to heal?
The initial phase of treatment for bone TB is to take the medication as prescribed by your doctor; this can take anywhere from twenty-four weeks to forty-two months to finish. When a patient exhibits any symptoms of bone TB, some of the most often prescribed medications are isoniazid, pyrazinamide, ethambutol, or rifampicin.
Does Bone TB Have a Complete Cure?
Bone TB is a very serious disorder because it kills the bone and deforms the thorax. It is crucial to recognize the symptoms of bone TB as soon as possible. Bone tuberculosis can be successfully treated if it is detected early. Understanding the disease and its symptoms is crucial.
Can Treatment Cause Bone TB to Recur?
You may contract tuberculosis again even though you have previously recovered from the illness. Remember that tuberculosis re-infection is becoming more common in the modern era.
Does Bone TB Spread?
In contrast to pulmonary tuberculosis, which can spread through breathing, bone tuberculosis cannot be spread unless a patient’s pus comes into contact with you. Diagnosing tuberculosis in the bone is extremely difficult because it may not show classic symptoms like a high fever or uncommon weight loss.
Reference
- Bone Tuberculosis | Narayana Health. (2020, February 20). Narayana Health Care. https://www.narayanahealth.org/blog/bone-tuberculosis/
- What Is Skeletal Tuberculosis? (2021, May 21). WebMD. https://www.webmd.com/lung/what-is-skeletal-tuberculosis
- Bone Tuberculosis: Symptoms, Causes, and Types | Metropolis TruHealth Blog. (n.d.). Metropolis India Lab. https://www.metropolisindia.com/blog/preventive-healthcare/bone-tuberculosis-causes-types-and-diagnosis
- Koprowski, B. (2023, June 9). What to know about bone tuberculosis. https://www.medicalnewstoday.com/articles/bone-tuberculosis#symptoms
- Crna, R. N. M. (2021, November 12). Tuberculosis. Healthline. https://www.healthline.com/health/tuberculosis#prevention