MYOSITIS OSSIFICANS (MO): PHYSIOTHERAPY MANAGEMENT
MYOSITIS OSSIFICANS (MO)
INTRODUCTION/DEFINITION:
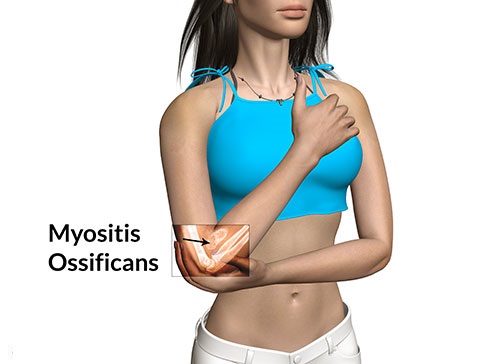
-
- Myositis ossificans results from a complication of a contusion injury and occurs when part of of the hematoma is replaced with bone. This condition can occur anywhere in the body but more commonly occurs in the quadriceps.
- The bone deposits may occur as a separate piece or pieces of bone lying entirely within the muscle or attached to the bone (exostosis).
- These calcium deposits are thought to be caused by periosteal cells that invade the hematoma following the injury.
- This causes a partial avulsion of muscle fibers from the periosteum.
MECHANISM OF INJURY:
- Usually caused by injuries that result in a severe contusion or chronic contusion injuries.
Patient will first present with severe pain at first usually with a contusion and a palpable mass within the muscle.
PATHOGENESIS OF MO:
- Muscle is commonly but not invariably involved, and fascia, tendon and periosteum can also be the site.
- Process is peculiar alteration within the ground substance of connective tissue, associated with striking proliferation of undifferentiated mesenchymal cells.
- Initially there is degeneration and necrosis, in case of muscle, disrupted muscle fibers retract. In 3 to 4 days, fibroblasts from endomysium invade damaged area and rapidly form broad sheets of immature fibroblasts.
- At the same time, primitive mesenchymal cells proliferate within injured connective tissue. Intense cellular proliferation of fibroblasts and mesenchymal cells produces a histological picture that may be erroneously diagnosed as fibrosarcoma or myosarcoma.
- Ground substance becomes homogeneous or glassy or waxy, suggesting some type of edema. It increases in amount and encloses some of mesenchymal cells, which then assume the morphological characteristic of osteoblasts. Mineralization follows and bone is formed. This events typically takes place first within least damaged part i.e. periphery.
- As the process of osteoid formation and mineralization changing in mature bone evolves, it progressively extends towards the central, severely damaged area. When myositis is not removed and is allowed to mature, it becomes oriented and covered by a cartilaginous cap, because of muscle action over the lesion. This is called post traumatic osteochondroma and is common in region of knee joint.
CAUSES:
- Contusions that are severe.
- Contusions resulting in a large loss of movement.
- Contusions that are inappropriately managed.
- Re-injury to the contusion (e.g. an additional impact).
- Patients who do not rest sufficiently following a contusion.
- Patients who do not use ice following a contusion.
- Patients who receive massage too soon or too vigorously following injury.
- Patients who exercise (e.g. stretch) or perform activities into pain.
- Patients who continue to play through injury.
- Patients who recommence sport too early following injury.
SIGNS AND SYMPTOMS:
- Restricted range of movement.
- Bruising.
- Pain.
- Palpable mass in muscle.
- An X-ray can show bone growth.
EXAMINATION AND EVALUATION:
- Observation.
- Look at how the athlete moves.
- Look for swelling, contusion, and ecchymosis.
- Check for a palpable mass within the muscle. Mass usually shows up within 2-3 weeks.
- Palpation.
- Palpate along the muscle and around the contused area to feel for a calcium deposit.
- Special Test.
- Manual Muscle Testing- assess the strength of the athlete you are testing.
- Check Range of Motion-check the athlete’s range of motion to see if calcium deposit is decreasing ROM.
DIFFERENTIAL DIAGNOSIS:
- There are three types of myositis ossificans:
- Type1: There is a thin stalk of bone formed between the ossified muscle and bone.
- Type2: A broad are of ossified muscle in located between muscle and bone.
- Type3: The ossified muscle is not connected to the bone, and even appears to derive completely from muscle.
DIAGNOSTIC PROCEDURE:
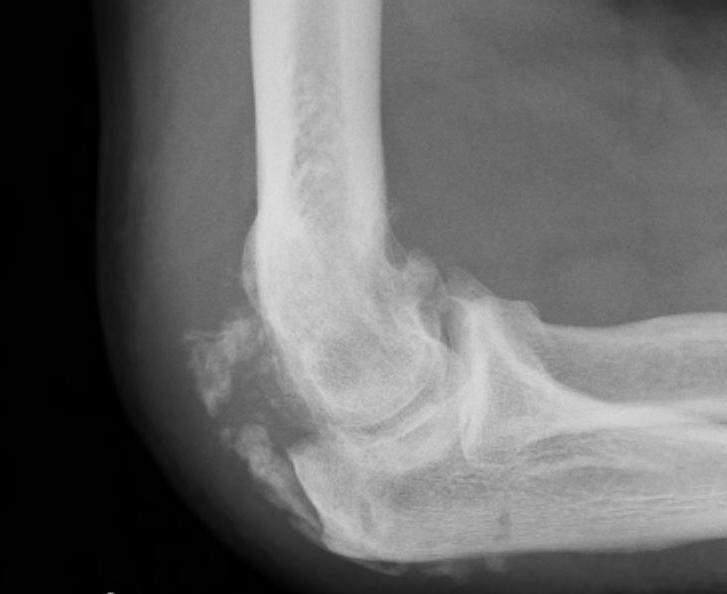
- Plain film radiographs.
- MRI.
- CT scan.
- Bone scan.
TREATMENTS OF MO:
- Rest.
- Immobilization.
- Anti inflammatory drugs.
- Physiotherapy management.
- Surgical debridement.
PHYSIOTHERAPY MANAGEMENT OF MO INCLUDES:
- Rest.
- Immobilization.
- TENS.
- Pulsed Ultra sound and phonophoresis.
- Maintain available range of motion but avoid stretching and massage, until maturation.
- Iontophoresis with 2 % acetic acid solution.
- Extra corporeal shock wave therapy.
- Pain free gentle ROM exercises.
- Cold therapy application- Elevation.
- Compression.
SURGICAL MANAGEMENT:
- Growth should not be removed in premature stage as it will likely reoccur.
- The ossification becomes exuberant, infiltrates beyond the original site, and compresses the soft tissues around beyond hope of repair.
- When after serial x-rays the mass is dense, well delineated, and at a stand still, it may be safely removed. It may be possible to prevent myositis by aspirating the original haematoma.


3 Comments